Prostate cancer is second most common cause of cancer related death in men next to lung cancer according to world literature.Though incidence of prostate cancer is reported to be less, common in Asians there is no data to confirm this.
The death rate from prostate cancer has decreased nearly 10% over past 15 years and indirect evidence for positive impact of screening strategies.
Prostate cancer occurs when cells in the prostate grow and multiply uncontrollably. The nodular tumour mass invades the surrounding tissues and eventually spread to the lymph nodes, skeletal bones and other regions of the body. The most common cancer in American men.
Early Detection
Your best chance for surviving prostate cancer is detecting it early. When prostate cancer is found early and treated appropriately, there is more than 90% chance for cure.
Symptoms
Early prostate cancer often have no symptoms. If symptoms are present, they vary from man to man, and may include:
- Frequent, difficult or painful urination
- Not being able to urinate
- Weak or interrupted urine flow
- Blood in the urine
- Blood in the semen
- Painful ejaculation
- Frequent pain or stiffness in the lower back, hips or upper thighs
Risk Factors
Many factors may influence the development of prostate cancer, including:
- Age Men 50 or older are at the greatest risk. Age is the most influential risk factor.
- Family history Your risk is higher with a family history of prostate cancer (especially father, brother, son)
- Diet A high-fat diet, particularly animal fats, may increase your risk. Diets high in fruits and vegetables are thought to decrease your risk.
Treatment
Surgery and Radiation are the two options available for the treatment of early prostate cancer.
Today Robotic Assisted Laparoscopic Prostatectomy is the gold standard in treatment of localized prostate cancer.
- Better preservation of continence
- Better preservation of sexual function
- Less complication
- Less blood loss
- Early return to work
- Less pain
Active Surveillance – Low risk prostate cancer can be managed by surveillance. It avoids the complications associated with surgery and radiation. Regular biopsy and MRI is needed as part of surveillance.
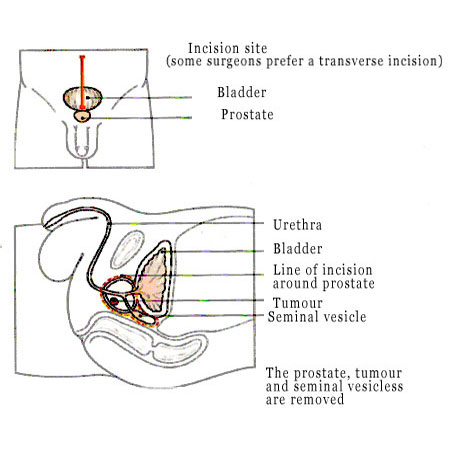
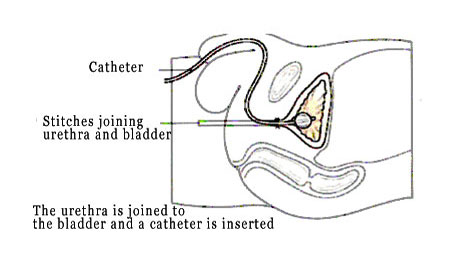
Radical Prostatectomy
Surgery may optimally treat prostate cancer if it has not spread outside the prostate. Surgery can be performed laparoscopic, retropubic or perineal. It involves the removal of the entire prostate and attached seminal vesicles, along with a small part of the bladder next to the prostate. Nerve sparing, whereby the surgeon identifies and leaves intact nerves either side of the prostate, can lower the risk of adverse affects following prostatectomy. Along with risks associated with any major surgery, adverse effects include impotence, urinary incontinence and urethral stricture.
Orchidectomy
Orchidectomy is used as a treatment for prostatic cancer, where it may be considered a form of hormonal manipulation. The surgical removal of both testes is performed via a small incision in the scrotum.
Hormonal Treatment
Hormonal treatment for prostate cancer also includes tablets or injections.
Chemotherapy is indicated certain cases of advanced prostate cancer.
 Urologist in Chennai | Robotic Urologist in India | Chennai Urology
Urologist in Chennai | Robotic Urologist in India | Chennai Urology