Lower urinary tract symptoms (LUTS ) includes
- Frequency-It is most common urological symptom. Normal adults pass urine 5 to 6 times a day.
- Urgency is inability to postpone urination
- Nocturia-Normal adults pass no more than twice at night to void.
- Dysuria-is painful urination often causing pain at the tip of the meatus.
- Decreased force of urination is usually due to obstruction commonly from benign enlargement of prostate or urethral stricture.
- Urinary hesitancy is delay in start of micturation.
- Intermittency is involuntary start-stopping of the urinary stream
- Straining is use of abdominal musculature to urinate
Severity of the problem is assessed by
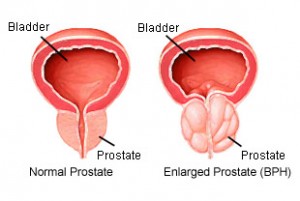
 Benign prostatic hyperplasia (BPH)
Benign prostatic hyperplasia (BPH)
Benign prostatic hyperplasia (BPH) refers to non-cancerous enlargement of the prostate with age. As the prostate enlarges the urethra gets ‘squeezed’ and narrows. This results in blockage of the passage of urine from the bladder and greater pressure is required to pass urine. BPH can also cause urinary incontinence, recurrent urinary tract infection, bladder stone formation, and occasionally kidney failure
Risk Factor
BPH rarely causes symptoms before age 40, but more than half of men in their sixties and as many as 90 percent in their seventies and eighties have some symptoms of BPH.
Causes
The cause of benign prostatic hyperplasia is unknown. It is possible that the condition is associated with hormonal changes that occur as men age.
Signs and Symptoms
Common symptoms of benign prostatic hyperplasia include the following:
- Pushing or straining to begin urination
- Hesitant, interrupted, or weak urine stream
- Dribbling after voiding
- Feeling that the bladder has not emptied completely after urination
- Frequent urination
- Urgency (sudden urgent need to urinate)
- Nocturia (needing to wake up to pass urine at night)
- Incontinence or leakage of urine
- Blood in the urine
In severe cases of BPH, acute urinary retention (sudden complete inability to urinate) can result from
- holding urine for a long time
- alcohol consumption,
- long period of inactivity,
- cold temperatures,
- allergy or cold medications containing decongestants or antihistamines,
- some prescription drugs (e.g., ipratropium bromide, epinephrine).
Diagnosis
- physical examination,
- patient history,
- evaluation of symptoms provide the basis for a diagnosis of benign prostatic hyperplasia.
- The physical examination includes a digital rectal examination (DRE), This exam reveals the size, shape, consistency of the prostate. In benign enlargement, the prostate is smooth, symmetrical and rubbery.
The PSA blood test is done to differentiate between BPH and prostate cancer.
- Urine flow study: It measures how quickly the urine is flowing. A reduced flow may mean you have
- BPH. Cystoscopy: This is an internal examination of urethra and bladder. The cystoscope is an instrument like a telescope, which is inserted through the urethra into the bladder. It allows to view the inside lining of the urethra, prostate and bladder.
- Prostate Ultrasound: To study the shape and volume of prostate and to diagnose prostatic disorders like prostatic cyst, abscess, calcification, enlargement and cancer.
- Ultrasound kidney: To study the size and shape of the kidneys and to diagnose kidney stones, tumours, cyst and obstruction.
How is BPH treated ?
Several treatments are available. Choice of treatment options will depend on age of patient, severity of BPH and general wellbeing of patient.
- Watchful waiting: If your symptoms don’t bother you too much.Have regular checkups and be ready to start treatment as soon as you need it.
- Medication: The alpha-blockers work by relaxing the prostate to keep it from blocking the bladder opening. Symptoms are relieved rapidly within a few days. It may cause some amount of giddiness especially if one gets up suddenly from a lying to a standing position. Symptoms usually reappear when the medication is stopped. The 5-alpha reductase inhibitors are used to shrink the prostate. It takes three to six months to shrink the prostate by about 20 to 30% in size. Symptom relief is slower and sexual function may be affected in up to 10% of patients.
Minimally Invasive Treatment
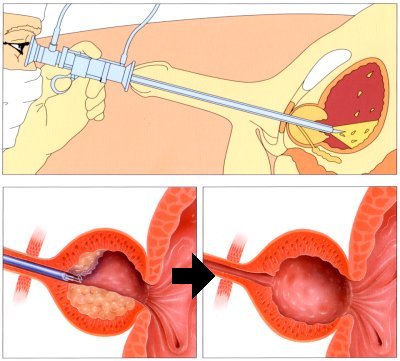
Minimally invasive BPH treatments use state-of-the-art tools and techniques to reduce or eliminate symptoms. The gold standard surgery for BPH is a TURP or transurethral resection of prostate. In TURP, the surgeon inserts a thin telescopic tube up the urethra and cuts away pieces of the prostate with a wire loop. By coring out the central enlarged and obstructing portion, a wide channel is obtained which will improve the urine flow and reduce symptoms dramatically. This procedure is painless under general or regional anesthesia.
TURP Transurethral Resection Of Prostate
In transurethral resection of the prostate, (a) the median lobe is resected
and (b) lateral adenoma tissue removed, leaving a cavity that
subsequently epithelializes over 4-6 weeks
Open Prostaectomy
Usually performed when the prostate is too large to be removed endoscopically.
TURIS
Recent advancement in treatment of BPH.
The limitation of TURP in treatment of large prostate if fluid absorption and consequence side effect. This is overcome when TURIS is used. It is special equipment where there are no side effects of fluid absorption. This allows
- Treatment of large glands with endoscopic method.
- Follow the conventional gold standard TURP
- No additional cost
- Reduces the side effects
HoLeP
Holmium laser enucleation of Prostate.
HoleP is minimally invasive treatment of choice for large prostate. Results are comparable to open prostatectomy.
 Urologist in Chennai | Robotic Urologist in India | Chennai Urology
Urologist in Chennai | Robotic Urologist in India | Chennai Urology

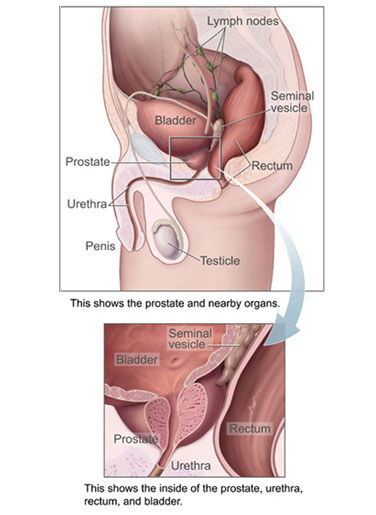 Benign prostatic hyperplasia (BPH)
Benign prostatic hyperplasia (BPH)